REGIONAL and rural patients have to travel an average of 122km to see a specialist, while more than half are waiting weeks or months to see a GP.
Subscribe now for unlimited access to all our agricultural news
across the nation
or signup to continue reading
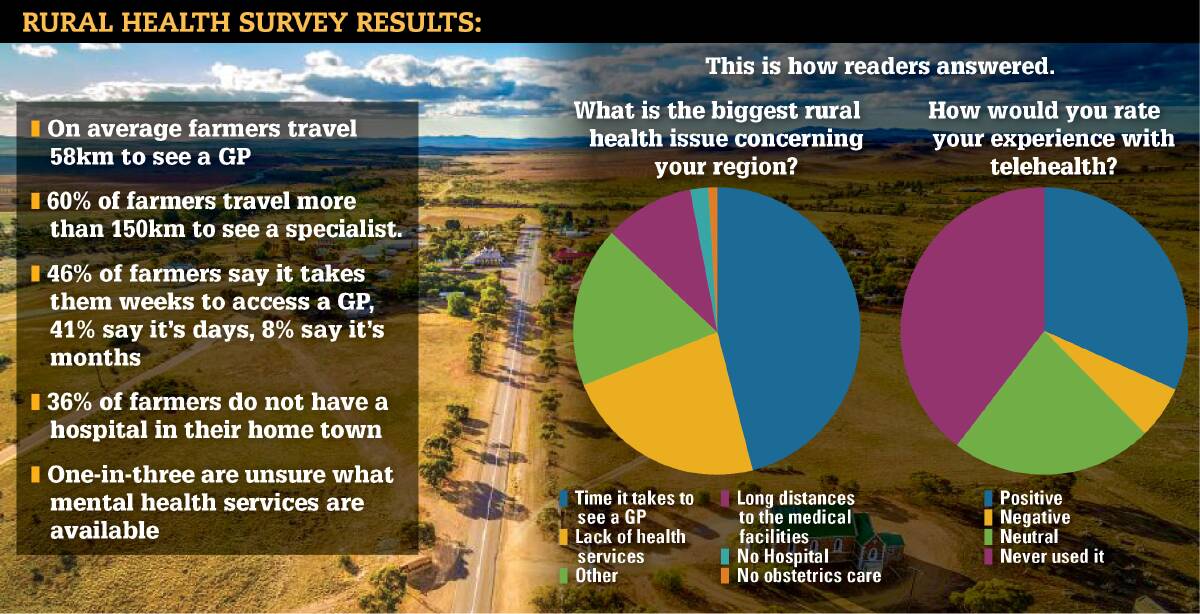
The grim findings of ACM rural health survey, which polled almost 2250 regional, rural and remote residents from across the country.
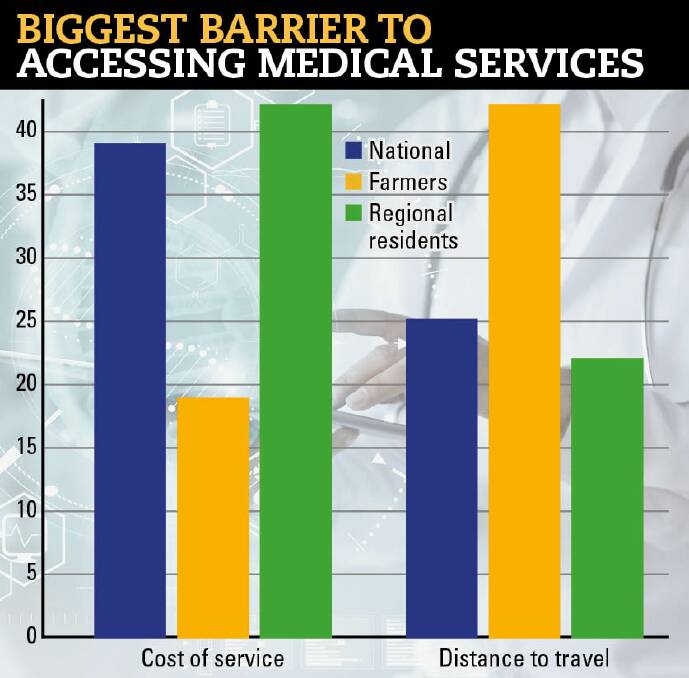
One-in-four regional residents, or 25 per cent, have to travel more than 150km to see a specialist and for farmers that figure jumped to 60pc.
Rural Doctors Association of Australia president and regional GP Megan Belot said the situation "extremely frustrating" to regional patients and their doctors.
"It can take a lot of effort and time to convince a patient to see a specialist because it's a six-hour round trip - and sometimes specialists send them back with just an appointment for a later date," Dr Belot said.
"We're very supportive of getting specialists out into the regions, even if it's just once a month."
Female farmers have to travel almost 100km on average to give birth, with one-third travelling more than 150km.
On average, farmers had to travel 58km to see their GP, with one-fifth travelling between 80 to 150kms.
Although frustrating, many regional patients are willing to make the long journey if it means they could see a doctor in a reasonable time frame.
Of those surveyed, 46pc said the biggest health concern in their region was the time it takes to access a GP appointment, 41pc of people had to wait days to see their doctor, while 46pc were forced to wait weeks.
Nationally, 8pc of people had to wait months, but in NSW one-third of regional residents were waiting months to see their GP.
Face-to-face consultations are the "gold standard" Dr Melot said, but there was definitely room to expand and promote the use of telehealth. A third had a positive experience with telehealth, a quarter had a neutral experience but 40pc had never used it.
"It really helps to supplement face-to-face appointments, and with the video option it makes follow ups easier for specialists and rural GPS, particularly with those long travel times," Dr Melot said.
In July, the federal government launched its Strengthening Medicare Taskforce to assess gaps in the nation's healthcare system, setting aside $750 million to implement the taskforce's recommendations.
Assistant Minister for Regional Health Emma McBride said there was strong rural and regional representation in the taskforce, which had been meeting monthly.
"We're listening to the health practitioners who live and work in those communities because different incentives have been tried in the past - and with good intention - but haven't led to a change in affordable access to care," she said.
Ms McBride, who was a regional pharmacist on the front lines giving people the jab during the COVID-19 pandemic, said the Commonwealth's timeline reflected the anxiety rural communities had about the state of their health services.
The recommendations from the taskforce are due at the end of the year and will be fed through the May budget process "to look at solutions that will make a difference, especially to people living outside of bid cities".
"There is a sense of urgency on the government's part to make sure there are solutions that are in place now and are sustainable into the future," Ms McBride said.
"We know that the further you live outside a major city, the worse your health outcomes are likely to be, and part of that is access to timely care - whether that's waiting day to weeks for your GP or travelling over 100kms to see a specialist."
A quarter of people surveyed by ACM said the lack of health services was the biggest issue in their region. Many respondents specifically highlighted the lack of mental health services, but one-in-three were also unaware of what services were available in their community.
Ms McBride said patients often had to access mental health services during a crisis and the system could be particularly difficult to navigate quickly.
"That's something that we're focused on as well is, making sure that services are available and how can someone navigate those services particularly if they're in distress or in crisis," Ms McBride said.
READ ALSO:


