
A new approach to employment could be the key to getting GPs into rural communities, as young doctors continue to shun the career path.
The Rural Doctors Association of Australia (RDAA) has thrown its support behind the Single Employer Model, in the hopes it could encourage more people to consider general practice or rural generalism.
While junior doctors enjoy salaried employment and leave entitlements during their time in the hospital system, the switch to private or community practice has often been a source of uncertainty for doctors wanting to train as a GP.
Under the Single Employment Model, GP registrars would be employed on a salary by an outside entity, rather than by the practice.
RDAA president Dr RT Lewandowski said it would provide the same level of security as doctors training in other medical specialities, who usually remained in the hospital system for a longer period.
"The vast majority of medical services in rural areas are provided by GPs and RGs, so the ongoing shortage of junior doctors wanting to train in these fields is a huge concern," Dr Lewandowski said.
"The complexity of employment arrangements, contract negotiations, loss of entitlements, and uncertainty around future income when training (which is fee-for-service based), have all been significant barriers for junior doctors in selecting a career in general practice."
For rural generalists, who often cover advanced skills such as obstetrics and anaesthetics in small hospitals, the situation is "more challenging".
In order to receive training both as a GP and in speciality hospital skills, junior doctors need to work across both a practice and the hospital system, meaning multiple contracts and often more uncertainty around income.
The Single Employer Model is set to be trialled in the NSW Hunter New England health district through 2024, initially in Tamworth and Armidale, after a pilot program in Murrumbidgee last year.
A trial of the model was also launched in rural communities across Tasmania last July, with a number of GP registrars remaining employed by the state government during their training.
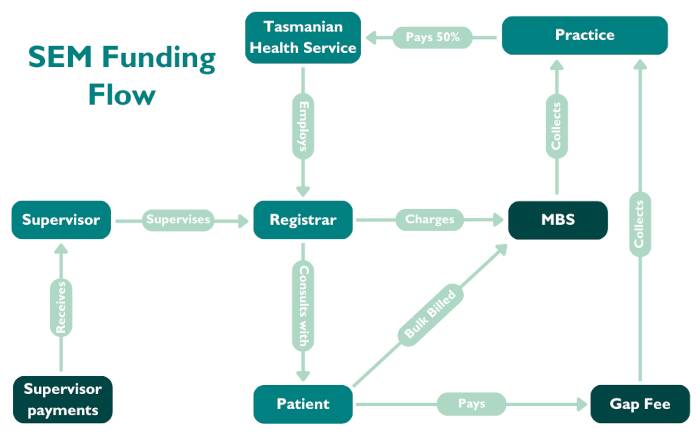
In lieu of registrars receiving a percentage of the billings, all their billings are collected by the practice and split with the health service to reimburse it for providing salaries.
The state and federal government are already in talks to increase the number of placements in the Tasmanian program this year, but the model has also faced criticism it might not be the right fit for every region.
A 2021 survey by the General Practice Supervisors Australia found only 18 per cent of its 400 members supported the model, believing it could limit the practice's control over leave and employment, impact income and performance, or disincentivise the relationship between registrars and the practice.
Some respondents also raised concern it would leave registrars unprepared when they finally entered the fee-for-service system and dealt with the private practice business model.


