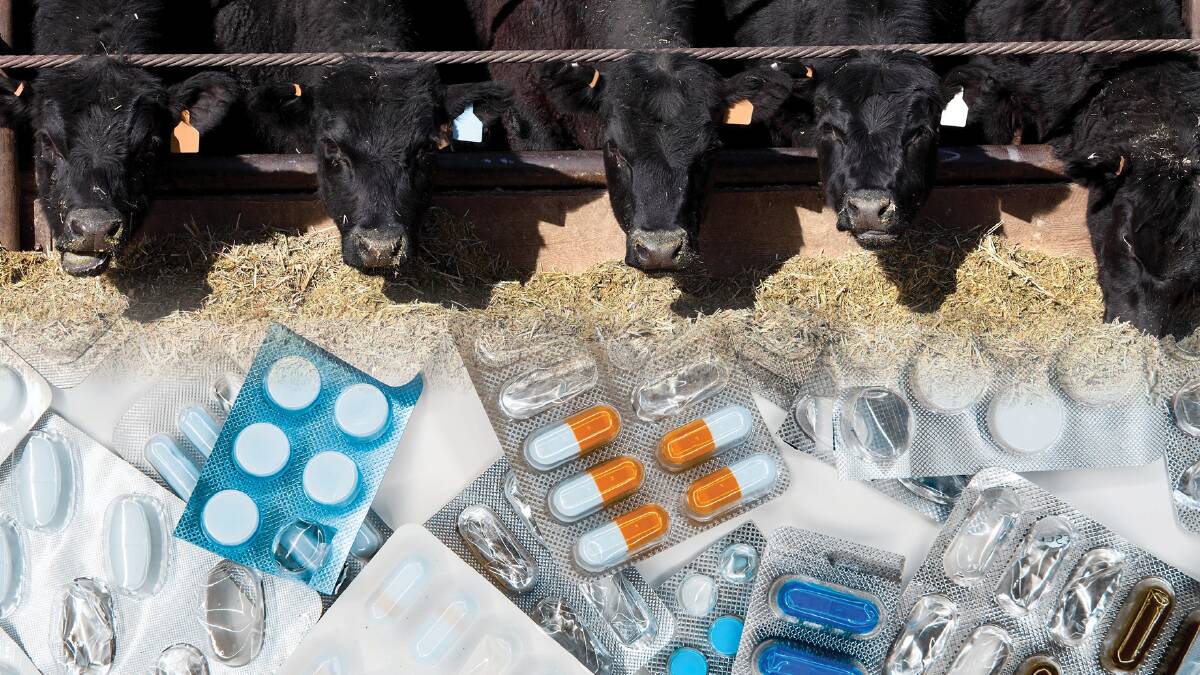
AS the world scrambles to avert a looming global health disaster from the rise of superbugs resistant to medicines like antibiotics, there are fears the impacts the crisis will have on food production are being overlooked.
Amid warnings of basic surgeries becoming too risky, ear infections deadly and simple rose thorn pricks in the garden leading to amputations, the idea that livestock production will be severely hamstrung without access to critical animal medicines barely rates a mention.
Yet the World Health Organisation warning, alongside its forecast that by 2050 the lack of effectiveness of common antimicrobial medicines will lead to 10 million people dying every year, is that it will also mean reduced food production, greater food safety issues and high economic losses to farm households.
A key issue is that not all global animal food producers are playing on the same field.
While Australia has minimised the use of antibiotics in food-producing animals to the extent that 99.9 per cent of its feedlots are now in compliance with strict antibiotic maximum residue limits, big animal meat producers like Brazil and China still have phenomenally high usage and, for some species, that is in fact increasing.
The Organisation for Economic Co-operation and Development says that is largely due to the impact on animal growth and profit margins on the farm.
Australia's beef industry clearly faces challenges to both stay competitive and play its part in tackling the crisis known as antimicrobial resistance.
Global burden
When bacteria, viruses, fungi and parasites change over time and no longer respond to medicines like antibiotics, antivirals, antifungals and antiparasitics, infections become harder to treat and the risk of disease spread, severe illness and death is increased.
This is antimicrobial resistance and it is occurring in people, animals and plants.
The global burden of deaths attributable to AMR is already 1.27 million a year - 5000 in Australia.
According to the CSIRO's famed report on global megatrends, Our Future World, AMR is now a more significant cause of death globally than malaria or HIV.
Solutions in the pipeline
CSIRO and the Australian Academy of Technological Sciences and Engineering, has just released a report looking at what Australia needs to do now to avoid being thrust back into a pre-antimicrobial age.
Branwen Morgan, lead of CSIRO's Minimising Antimicrobial Resistance Mission, said Australians could no longer take antibiotics for granted.
"It's not as simple as making new drugs to replace those that are failing," Dr Morgan said.
"Producing new antibiotics is a slow and expensive process and there is a high failure rate.
"And any new drugs will now be prescribed sparingly. The side effect of that is lower sales and very little return on the millions in investment in R&D.
"Therefore, an holistic approach is required that involves protecting the efficacy of the medicines we currently have and finding new solutions we can deploy as soon as possible."
From surface sprays that change colour when pathogens are present to neutralising technologies built into sewerage systems and toilets that detect and disarm harmful microbes before they reach our waterways, there are many innovations coming down the pipeline.
Even toothbrushes that self sterilise after use.
ATSE fellow Sue MacLeman listed integrated surveillance and sensing solutions to monitor AMR, point-of-care diagnostics to enable timely treatment of infections, new vaccinations and air sterilisation as key solutions.
Prevention through design of high-risk infrastructure like hospitals and farms would also be important, she said.
What Australian beef is doing
Australia has one of the most conservative approaches to antimicrobial use in the world, and is a world leader in minimising the use of antibiotics in food-producing animals, the Department of Agriculture says.
Antimicrobial stewardship is one of the six key priority areas identified in the Australian Beef Sustainability Framework, alongside the likes of managing climate risk and balancing tree and grass cover.
The Australian cattle feedlot industry was one of the first to release antimicrobial stewardship guidelines in 2018, which became mandatory from January 2022.
In addition to promoting the adoption of stewardship practices, the industry supports improved monitoring of use and surveillance of resistance to help inform policy and practice which is part of the broader strategy to reduce the risk of antimicrobial resistance.
ALSO SEE: Feedlot research ramped up to target AMR
The OECD says with the growing awareness of AMR, many countries have phased out the use of antimicrobials for animal growth promotion and are focusing on optimising their use in preventing and treating animal diseases.
"There is a common perception among producers that the benefits of antibiotics outweigh the costs but this depends on several factors, especially the biosecurity standards on the farm, housing standards, nutrition, breeding and management of the farm," the OECD said.
"In the long run, however, the negative spillover effects of antibiotic resistance on human health, as well as on animal health, can have major social, economic and environmental impacts.
"Finding the level of antimicrobial use that optimises the economic and technical performance on animal farms is a major challenge."
Bacteria in food supply chain

At Western Australia's Murdoch University, cutting-edge work pinpointing the level of AMR in beef, pork and chicken is underway.
Professor of Microbiology Sam Abraham is leading laboratory analysis to isolate bacteria from the meat and subject it to antimicrobial susceptibility testing.
Whole genome sequencing of selected bacteria is being used to detect genetic antimicrobial resistance determinants.
Professor Abraham said food sits at the interface between humans, animals and the environment.
"We all know that bacteria can be spread between people by coughing, sneezing, or direct contact, but what is often forgotten is that this same bacteria can also be passed on to companion animals, wildlife and livestock," he said.
"In addition, production animals and crops can move bacteria through the food supply chain, people can transfer bacteria to food during preparation, and our waste can contaminate soil and water, which in turn, can spread bacteria back to humans.
"This means AMR bacteria travels full circle, and the more we use antibiotics, the more AMR bacteria will be in that cycle."


