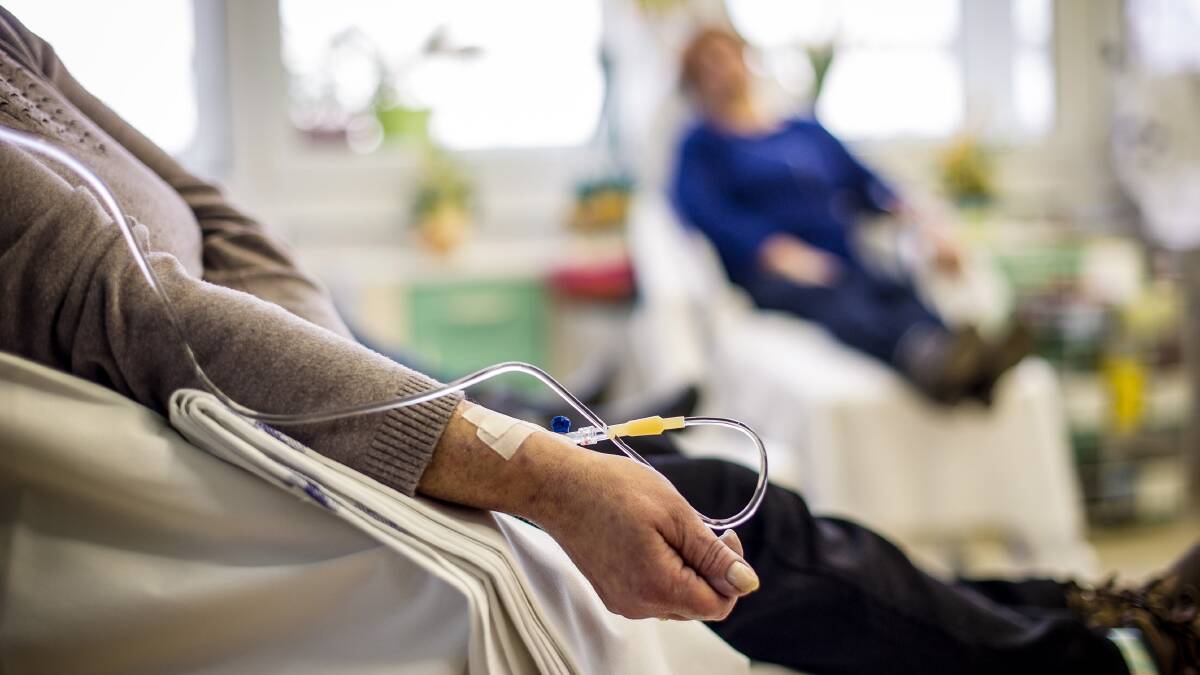
Regional Australians miss out on nearly $850 a year in healthcare access, which equates to a total annual rural health spending deficit of $6.5 billion, a new report has found.
Subscribe now for unlimited access to all our agricultural news
across the nation
or signup to continue reading
The National Rural Health Alliance, who commissioned the report, said the damning document provided clear evidence for the need to bring the country's scattered rural health initiatives under one umbrella.
Tweaking around the edges with trials and funding that stops after three years wasn't enough, NRHA chief executive Susi Tegen says. The regional primary health care system had to be redesigned at the grassroots level.
"Over 7 million people, who make up nearly a third of Australia's population, experience a greater burden from illness and early death, in part due to inadequate funding for their health care," she said.
"Why should people living in rural Australia pay twice or thrice the amount for the same health care available in cities, yet still have poorer health? This is the unfortunate reality faced by many rural Australians."
The report also highlights the way health services are funded and delivered are designed for metro populations and healthcare systems, and simply don't work in the bush.
National Farmers' Federation president Fiona Simson said if a national rural health strategy wasn't on the agenda at the next National Cabinet meeting, "we need to be asking serious questions of our leaders and their commitment to the regions".
"We have all been aware of the significantly worse health outcomes for rural Australians for some time," Ms Simson said.
"Which makes it concerning we have no current nationally agreed strategy bringing together a range of innovative models, funding structures and incentives to address this unacceptable disparity in health outcomes between Australians."
The NRHA, which represents 48 major regional organisations, said investing in rural health would have the additional benefit of reducing costs to hospital and emergency departments.
Health Minister Mark Butler said the government's recent healthcare measures would benefit regional patients, pointing to a $6.1b investment to strengthen Medicare and a $3.5b bulk billing incentive.
"Doctors' groups have called this a game-changer and GPs right around the country have said this will help them maintain and even shift back to bulk billing," Mr Butler said.
"On top of the investment in bulk billing, we are investing in a $1.5 billion indexation boost to every single Medicare rebate, increasing the amount that doctors receive for each Medicare service and reducing pressure on GPs.
"This increases rebates more in a single year than the former government did in seven years."


